The Senior Care Policy Briefing covers important long-term care issues by highlighting policy updates, news reports, and academic research.
Read the full Senior Care Policy Briefing below or download here.
November 30, 2023.
NEWSFLASH
- Nursing homes meeting CMS’s proposed staffing standards – which are dangerously inadequate – demonstrate higher overall quality ratings, lower likelihood of serious issues, fewer deficiencies in care, and reduced instances of patient abuse compared to those with lower staffing levels, according to a congressional analysis based on CMS data. The report, “Residents at Risk,” emphasizes the potential significant benefits of implementing the proposed standards but recommends finalizing a stronger version of the rule.
- The Office of Inspector General (OIG) found that CMS failed to use claims data to identify potential cases of neglect and abuse in Medicare patients, as reported by McKnight’s. OIG’s report revealed that an astounding 93 out of 100 sampled medical records showed evidence of potential abuse or neglect, as indicated by specific diagnosis codes.
LTC BY THE NUMBERS
- Cracking Down. The Department of Justice (DOJ) issued its annual report to Congress on its efforts to combat elder fraud and abuse. The report identified almost 300 criminal and civil actions against over 650 individuals for collectively stealing more than $1.5 billion from over 2.4 million adults, including assisted living residents, according to McKnight’s. The DOJ’s report highlighted various fraud schemes, including lottery, romance, and tech support scams, as well as pursuing nursing home operators providing substandard care.
- Occupancy Bounces Back. Though industry lobbyists claim that this is not the time for improved staffing or quality assurance, their own consultants report that, “Senior living occupancy could reach pre-pandemic levels next year.”
- The National Investment Center for Seniors Housing & Care reports nine consecutive quarters of occupancy recovery, driven by “record-high” rates of demand.
GET THE FACTS
- Negligence Unchecked. In 2021, an assisted living resident in Maine died after suffering a severe allergic reaction to a peanut butter sandwich. Despite the resident’s documented allergy, an employee served him the sandwich. Following an investigation, the Maine Department of Health and Human Services issued two citations for resident rights violations. The health department had the authority to impose fines or issue a conditional license (which bars facilities from accepting new residents for up to 12 months) but opted for a corrective plan from the facility. Takeaway: The failure of oversight agencies to impose meaningful penalties allows poor conditions to persist in nursing homes, posing risks to vulnerable residents.
- “What’s the impetus to change if there’s no consequence?” -Paula Banks, Geriatric Care Manager, via ProPublica
THE COST OF LIVING
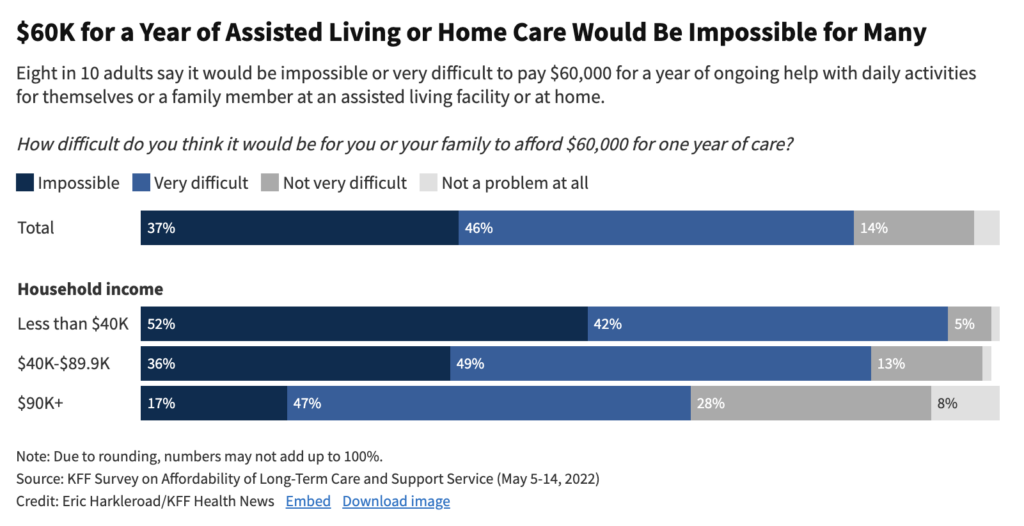
Assisted living facilities (ALFs) are often financially out of reach for most Americans. These facilities, housing around 850,000 older Americans, charge $5,000 a month or more, with additional fees for various services. Investors and real estate investment trusts have found ALFs to be a lucrative branch of the long-term care industry, with half of operators earning returns of 20% or more. Chart via KFF.