The Senior Care Policy Briefing covers important long-term care issues by highlighting policy updates, news reports, and academic research.
Read the full Senior Care Policy Briefing below or download here.
October 15, 2023.
NEWSFLASH
 About a Dollar a Day. That’s the cost, per resident, that nursing homes would need to pay to meet the 24-hour RN requirement in CMS’s proposed minimum staffing standards. LTCCC’s new analysis finds that the annual cost to meet the 24-hour RN standard costs only $71 million – a fraction of the $610 million cost industry leaders claim.
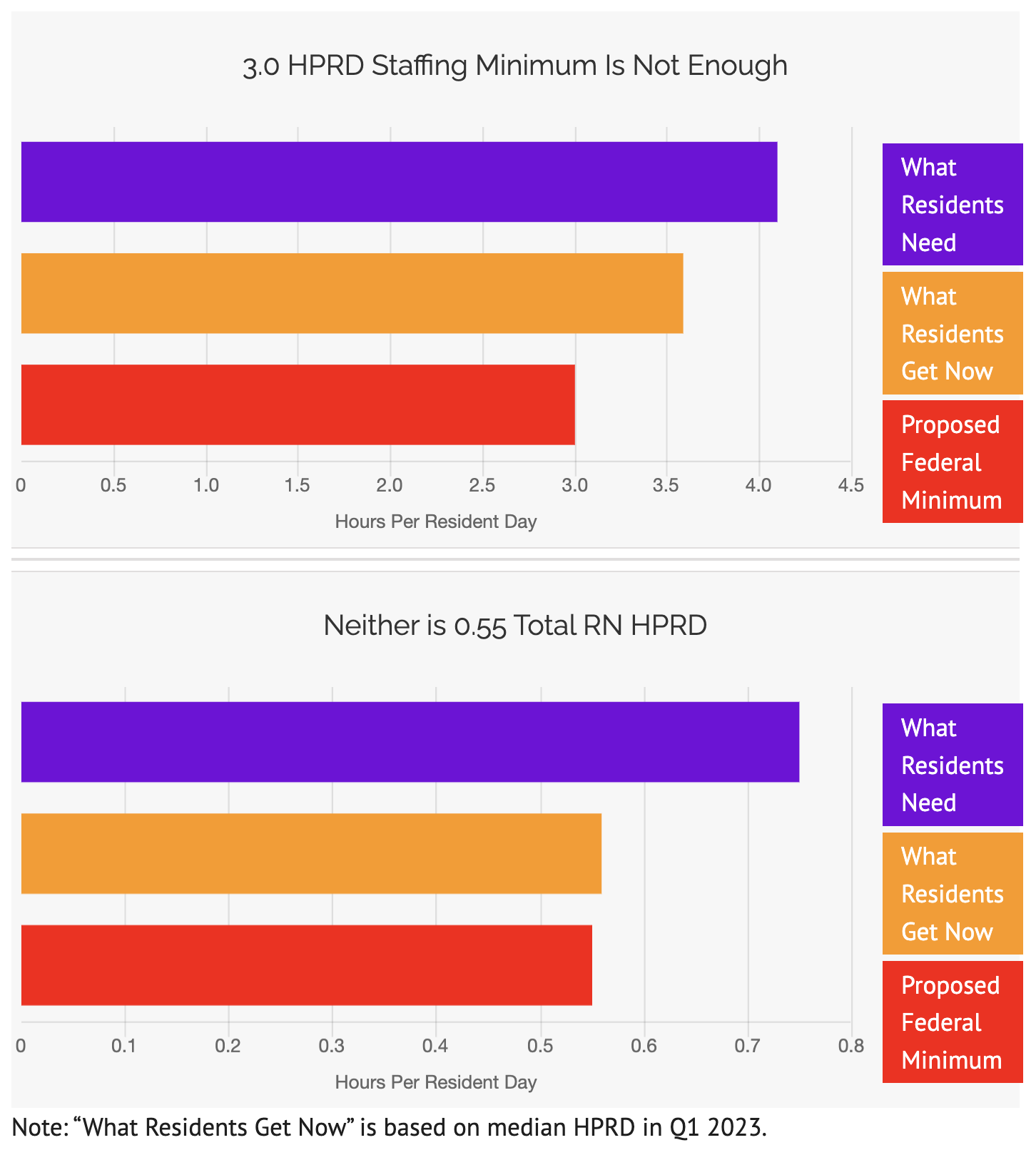
About a Dollar a Day. That’s the cost, per resident, that nursing homes would need to pay to meet the 24-hour RN requirement in CMS’s proposed minimum staffing standards. LTCCC’s new analysis finds that the annual cost to meet the 24-hour RN standard costs only $71 million – a fraction of the $610 million cost industry leaders claim.- 3.0 is NOT enough. Nursing home residents need 4.1 nurse hours per resident day (HPRD) to receive sufficient clinical care and avoid unnecessary harm, according to a landmark federal study. CMS’s proposed minimum of 3.0 HPRD could result in many facilities decreasing staff. It must be increased. Residents deserve better.
- A New Resident Population. Assisted living lobbyists often fight safety and staffing standards while at the same time acknowledging that “[t]he level of needs of older adults moving into assisted living communities today is similar to that of seniors who would move into nursing homes in the past.”
LTC BY THE NUMBERS
- A neurology-focused program aimed at reducing antipsychotic drug (AP) usage in nursing homes resulted in a 68% decrease in usage among individuals with behavioral and psychological symptoms of dementia. Additionally, it identified diagnostic corrections for 35% of the residents in the study, indicating that many had previously been misdiagnosed with conditions like schizophrenia rather than dementia.
GET THE FACTS
- Nursing home REITs (Real Estate Investment Trusts) offer attractive investment opportunities, especially given the aging population. However, research indicates that “[s]eparating real estate from care operations… poses serious risks and dangers for patient care.” The absence of strong staffing and financial accountability standards incentivizes operators to reduce care and maximize profits.
- Though lobbyists claim that this isn’t the time for safe staffing standards, the senior living sector is expected to see a strong recovery over the next 12 to 18 months, potentially outperforming the rest of the real estate sector.
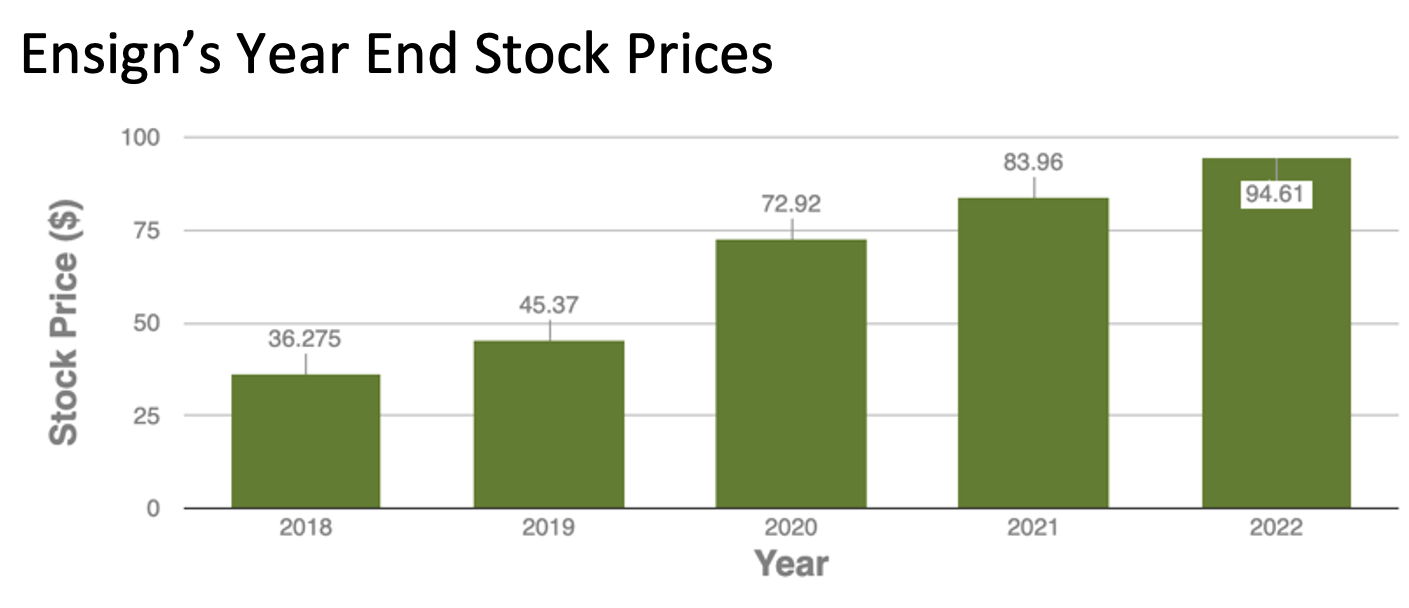
The Ensign Group is a large, multi-state nursing home chain. Ensign nursing homes have slightly lower nurse staffing levels (especially in RN staffing) and their COVID-19 outcomes were slightly worse or on par with the national average. Despite this, stock prices continue to climb year after year. It seems that Ensign prioritizes investors over nursing home residents.