The Senior Care Policy Briefing covers important long-term care issues by highlighting policy updates, news reports, and academic research.
Read the full Senior Care Policy Briefing below or download here.
May 15, 2026.
NEWSFLASH
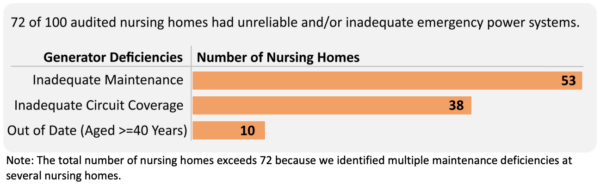
- A new HHS Office of Inspector General report found that most nursing homes in the United States do not have adequate or reliable emergency power systems, putting residents at serious risk during disasters and power outages. Auditors estimated that 73% of nursing homes nationwide have emergency power deficiencies, including inadequate generator maintenance, insufficient circuit coverage, or aging generators. The report warns that these failures increase the risk of injury or death during emergencies such as hurricanes, winter storms, and heat waves.
- Three affiliated skilled nursing facilities have agreed to pay $300,000 to resolve False Claims Act allegations related to alleged failures to provide required services to residents while billing federal healthcare programs. According to the Justice Department, the case involved concerns that residents did not receive the level of care mandated under federal requirements despite facilities seeking reimbursement. The settlement adds to ongoing federal scrutiny of nursing home compliance and billing practices.
INDUSTRY NEWS
- Nursing home industry representatives are celebrating recent regulatory “improvements” that they say will “streamline regulations and support providers.” Industry leaders and lobbyists argue that the updates will improve efficiency and help facilities focus more resources on operations and care delivery.
- Calls to “streamline” regulation come at a time when audits, enforcement actions, and research continue to document serious problems in nursing homes, including understaffing, inaccurate reporting, misuse of public funds, and resident harm. Numerous studies, including LTCCC’s 2022 analysis of national enforcement data, have found that many facilities openly flout even the most basic minimum standards with impunity.
- A new study found that nearly half of nursing home staff turnover may be going unreported, raising concerns about the accuracy of publicly reported workforce data, McKnight’s reports. Researchers found discrepancies between reported staffing information and payroll-based data, suggesting that turnover rates at some facilities may be significantly higher than disclosed. The findings call into question the reliability of staffing metrics used by regulators, consumers, and policymakers to assess nursing home performance.
- Underreported turnover can obscure the true extent of staffing instability in nursing homes, making it harder to identify facilities struggling to maintain a consistent workforce and potentially masking risks to resident care and safety.
- A new investigation found that lower nurse staffing levels in skilled nursing facilities are associated with longer hospital stays, suggesting that nursing home staffing shortages can have ripple effects across the broader healthcare system. Researchers found that a decrease of one nurse staffing hour per patient-day in local nursing homes was associated with a 3.5% increase in hospital length of stay.